At one moment, you’re juggling the responsibilities of work, relationships, finances, and family all at once –– and all the stress that comes with that balancing act. Then suddenly, you realize you’ve shut down and you’ve lost the motivation to keep all your plates spinning.
If this sounds familiar, you may be emblematic of a possible trend that scientific research has been exploring for years. Experts believe there is a connection between chronic stress and the development of depression.
A new kind of depression?
There are a number of different categories of depression, according to beyondblue, an Australian nonprofit devoted to mental health support. Melancholia, psychotic depression, and postpartum depression are all under the umbrella of major depression (MD), which is sometimes called major depressive disorder or shortened to simply “depression.” To be diagnosed with clinical depression, doctors consider if patients have exhibited symptoms daily for at least two weeks, according to WebMD. These symptoms can include sadness, loss of interest in activities they previously enjoyed, insomnia, difficulty concentrating, hopelessness, fatigue, and suicidal thoughts.
In their paper “Stress and Depression: Preclinical Research and Clinical Implications,” researchers Alessandro Bartolomucci, PhD. and Rosario Leopardi say the evidence for stress as a causal factor is growing. Because of this, they name “stress-induced depression (STRID)” as its own category. They say they’re not the first experts to use the term, but they qualify STRID as a “temporary” subtype of MD until more psychologists can confirm it.
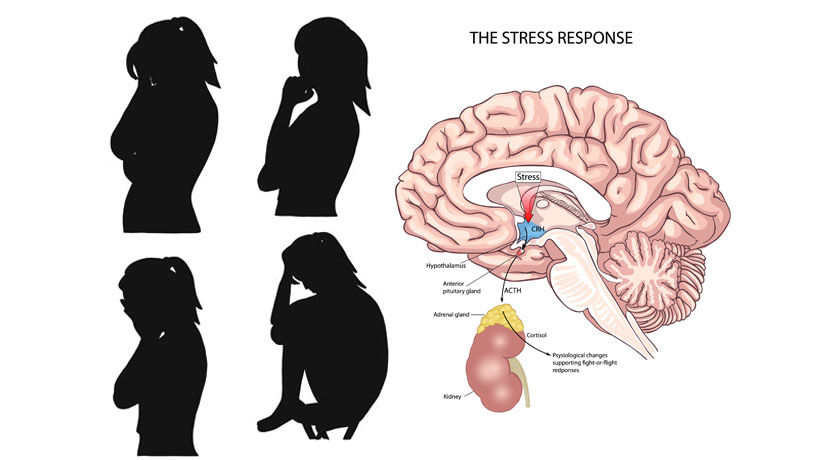
Stress, depression, and the brain
Harvard Health Publishing found evidence that the hippocampus, the part of the brain responsible for emotion, is generally smaller in depressed people. Stress may contribute to this because because experts believe exposure to cortisol impairs the growth of new neurons in the hippocampus.
This idea was echoed by a 2015 paper published in Current Neuropharmacology. “Chronic stress exposure induces reduced hippocampal volume and diminished expression of neurotrophic factors,” they write, “and inhibits neurogenesis occurring in dentate gyrus in the adult brain.” The authors of the paper then suggest the stress-induced changes in the brain could be reversed by antidepressants.
Hormonal change
According to the study “Can stress cause depression?” by H.M. van Praag in the World Journal of Biological Psychiatry, stress might cause major depression because of a change of hormonal production. This study focused on the 5-hydroxytryptamine receptors (5-HT) receptors, which are serotonin receptors. Serotonin is a chemical that helps regulate mood, sleep, and memory. Experts link low serotonin levels with depression, which is why serotonin receptors are the target for antidepressants.
Van Praag determined stress could cause brain disturbances associated with certain kinds of depression. He suggested changes in the 5-HT and stress hormone systems produced by stress are similar to hormonal changes in depression.
Behavioral influence
While science develops more evidence to confirm the way stress affects depression in the brain, there may be stress-induced behaviors that have a relationship with depression. Alice Boyes, Ph.D wrote in Psychology Today that stress can cause unhealthy coping habits. For example, a routine of excessive alcohol use during a stressful period can lower your mood or affect sleep, which are symptoms of depression. Another example is overworking on a project and running out of time for exercise and sleep.
Doctors are more likely to diagnose patients with depression who have a genetic predisposition for the mental illness, so just because you’re suffering from stress doesn’t mean you are guaranteed to have the mental illness. However, managing your stress in a healthy way might help prevent the onset of depression.
Sources:
https://www.beyondblue.org.au/the-facts/depression/types-of-depression
https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0004265
https://www.webmd.com/depression/guide/depression-diagnosis#1
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4790405/
https://www.health.harvard.edu/mind-and-mood/what-causes-depression
https://www.ncbi.nlm.nih.gov/pubmed/16166019
https://pubs.acs.org/doi/abs/10.1021/cr078224o
https://www.psychologytoday.com/us/blog/in-practice/201303/why-stress-turns-depression